|
||||||||||||||||||||||||||||||||||||
| [
Contents
] [ INDEX ]
|
||||||||||||||||||||||||||||||||||||
|
Page 6 |
||||||||||||||||||||||||||||||||||||
|
Original paper Rotational thromboelastometry guided blood component administration Radovan Dinić (1), Almira Šabani (1), Jasmina Grujić (2) 1) HOSPITAL BLOOD BANK, DEPARTMENT OF PRE-TRANSFUSION TESTING, EMERGENCY CENTER OF THE UNIVERSITY CLINICAL CENTER OF SERBIA, BELGRADE; 2) DEPARTMENT OF TRANSFUSIOLOGY, FACULTY OF MEDICINE, UNIVERSITY OF NOVI SAD, NOVI SAD |
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
| Download in pdf format | Abstract:
Introduction: Rotational thromboelastometry is a diagnostic tool
extensively utilized for patients at high risk of bleeding,
particularly those experiencing trauma or undergoing significant
surgical procedures. This test is notable for providing rapid
results, facilitating timely decisions regarding the application of
individualized transfusion therapies, thereby optimizing the
rational use of blood components. Aim: The objective of this
study is to assess the utilization of blood components in the
transfusion treatment of patients at the Emergency Center of the
University Clinical Center of Serbia, based on the outcomes of
rotational thromboelastometry. The analysis aims to evaluate the
frequency of these interventions in the studied population and to
highlight the advantages of this treatment modality. Material and methods: This retrospective study analyzed trauma patients who underwent rotational thromboelastometry at the Hospital Blood Bank, Department of Pre-transfusion Testing, Emergency Center of the University Clinical Center of Serbia, from January 1st 2023, to December 31st 2023. Data regarding the results of the thromboelastometry tests and subsequent blood component therapies were extracted from the Service's protocols. Results: During the study period, 776 patients were evaluated by means ofrotational thromboelastometry, of which 358 (46.13%) required blood component therapy. Cryoprecipitate was administered to 48 (13.40%) patients, platelet concentrate to 69 (19.27%), and a combination of cryoprecipitate and platelets to 61 (17.03%) patients. Additional therapeutic approaches included the administration of platelets, desmopressin, and tranexamic acid, while fresh frozen plasma was utilized the least, in only 17 (4.74%) patients. Conclusion:The analysis of blood components used for therapeutic purposes in relation to the rotational thromboelastometry demonstrated a wide range of therapeutic modalities in the treatmentof patients. This testing method facilitates individualized therapy with blood components, subsequently diminishing the needfor transfusions, enhancingallows for better diagnostic precision, and reduces costs associated with long-term managementof patients. Key words: rotational thromboelastometry, therapy, trauma, transfusion, bleeding |
|||||||||||||||||||||||||||||||||||
|
INTRODUCTION Rotational thromboelastometry (ROTEM) is a test whichis an integral part of "Point-of-Care" testing. It is characterized by being performed within a short time frame after the patient's sample is taken, allowing timely decisions regarding the transfusion management of the patient. The results are obtained quickly, which enables a rapid modification of therapy if needed [1]. ROTEM testing is being increasingly integrated into the routine diagnostic algorithm and management of bleeding in patients at high risk of bleeding, such as trauma patients. At the Emergency Center of the University Clinical Center of Serbia, the majority of patients are those admitted urgently as a result of trauma. A rapid clinical assessment of the injured patient's condition allows the prediction of trauma-induced coagulopathy (TIC) and the need to activate the massive transfusion protocol [2]. For these purposes, multiple ROTEM tests can be used to distinguish between mechanical and hemostatic bleeding, identify disorders in various stages of the hemostatic process, thereby enabling targeted and rational use of blood and blood components. ROTEM is a functional test that graphically displays the formation and breakdown of a clot, allowing monitoring of the progression or resolution of coagulopathy following a trauma [3]. ROTEM screening tests Additional ROTEM tests The parameters of ROTEM analysis
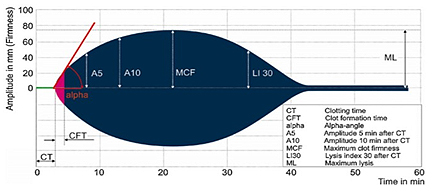
AIM The aim of this study is to assess the utilization of blood components in the transfusion treatment of trauma patients at the Emergency Center of the University Clinical Center of Serbia, based on the outcomes of rotational thromboelastometry. The analysis aims to evaluate the frequency of these interventions in the studied population and to highlight the advantages of this type of treatment for patients. MATERIALS AND METHODS This retrospective study analyzed trauma patients who underwent ROTEM testing in the Hospital Blood Bank, Department of Pre-Transfusion Testing, at the Emergency Center of the University Clinical Center of Serbia, from January 1st 2023, to December 31st 2023. Based on the obtained results, therapy was administered to each patient. Testing on the ROTEM analyzer was conducted using a tube containing 3.2% sodium citrate as an anticoagulant (Vacutainer Brand, Belliver Industrial Estate, Plymouth, UK, 4.5 ml, 9 NC 0.129 M). A volume of 300 µL of resuspended blood was taken from the tube for each of the two tests (EXTEM and FIBTEM) using a pipette with predefined aspiration and expiration time intervals, it was placed into the "cup & pin" chamber where specific activators for each test were added. Upon activation of each test, the results were monitored on the ROTEM analyzer screen (Figure 1), and once the values were obtained, the result was printed, described, and distributed along with the proposed therapy to the departments that had requested the procedure. Figure 1. Illustration of the ROTEM
graphical record showing all phases of hemostasis.
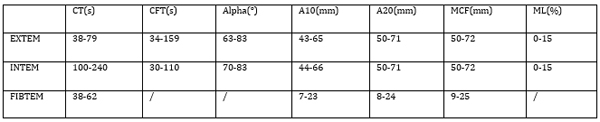
Table 1 presents the ROTEM reference values,on the basis of which the therapy was administered to patients. Table 1. ROTEM parameters, normal values
RESULTS During the observation period, ROTEM testing was performed on 776 patients. Based on the obtained results, 358 of them (46.13%) required therapy with blood components, while 418 (53.87%) did not need such therapy (Table 2). Table 2. Need for component therapy based on ROTEM parameter values
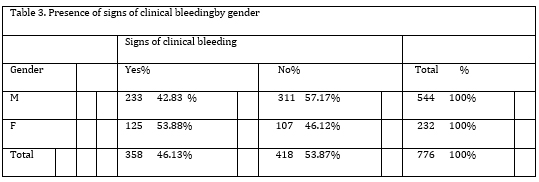
The occurrence of clinical bleeding in patients by gender is shown in Table 3. There is a statistically significant difference in the presence of clinical bleeding related to gender(Χ² = 7.989, p=0.005). Among female patients, 53.88% exhibit clinical bleeding, while 43.83% of male patients show signs of bleeding.
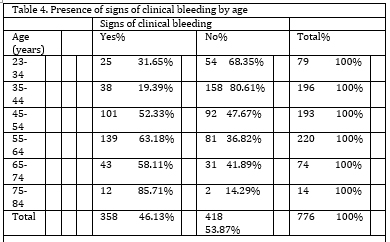
The occurrence of clinical bleeding in patients by age is shown in Table 4. There is a statistically significant difference in the presence of signsofbleeding based on the results of the Χ² test (Χ² = 104.902, p<0.001). Bleeding was most prevalent in the age group of 75 to 84 (85.71%) and least prevalent in the age group of 35 to 44 (19.39%).
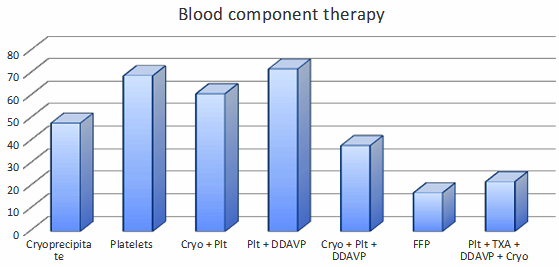
The distribution of blood component usage among patients is shown in Figure 2. Observing the distribution of blood components, we can see that cryoprecipitate was administered to 48 patients (13.40%), platelets to 69 patients (19.27%), and cryoprecipitate and platelets simultaneously to 61 patients (17.03%). The administration of platelets and desmopressin (DDAVP) was necessary for 72 patients (20.11%). Fresh frozen plasma (FFP) was used in only 17 patients (4.74%). A combination of platelets, tranexamic acid (TXA), DDAVP, and cryoprecipitate was administered to 22 patients (6.14%), while cryoprecipitate, platelets, and DDAVP were given to 38 patients (10.6%). Figure 2. Administered Blood Component Therapy
In 31 patients (8.65%), a tendency towards hypercoagulability was confirmed, and in 11 of these patients (35.48%), the administration of Kybernin P 500 was recommended as a substitution for antithrombin deficiency. DISCUSSION The aim of
this study was to assess the impact of ROTEM-guided transfusions on
the use of blood components in traumapatients. ROTEM-guided therapy
with blood components is associated with improved patient outcomes,
particularly as it also reduces the need for allogeneic blood
transfusions. Our study had a significantly higher proportion of
male patients (70.1%) compared to females. Gender differences among
trauma patients have been well documented in various studies, with a
higher prevalence of males. Specifically, men are more frequently
represented as polytrauma patients, often due to risky behaviors
that include alcohol consumption and driving under the influence of
alcohol [1]. Additionally, most causes for multiple injuries are
indeed the result of traffic accidents and work-related injuries,
which often occur in younger male populations who are more mobile
and engaged in physically demanding jobs [1,2]. Moreover, traumas
also occur among the elderly because of falls and fractures [1,3]. CONCLUSION The analysis of blood components used for therapeutic purposes guided by the rotational thromboelastometry demonstrated a wide range of therapeutic modalities in patient treatment. This testing method facilitates individualized therapy with blood components, subsequently diminishing the necessity for transfusions, enabling betterdiagnostic precision, and reducing costs associated with long-term patient management. Further studies and integration into standard clinical practices are warranted to enhance its effectiveness in patient care optimization and coagulopathy management. REFERENCES:
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
| [
Contents
] [ INDEX ]
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||