|
||||||||||||||||||||||||||||||||||||
| [
Contents
] [ INDEX ]
|
||||||||||||||||||||||||||||||||||||
|
Page 17 |
||||||||||||||||||||||||||||||||||||
|
Original paper Correlation of psychotic disorders with alcohol and other psychoactive substances abuse Nevena Đumić (1), Jovan Milatović (2), Ana-Marija Vejnović (2), Radoslav Pejin (3), Tamara Popović (2), Boško Čuturić (2) (1) MEDICAL FACULTY, UNIVERSITY OF NOVI SAD,NOVI SAD; (2) PSYCHIATRY CLINIC, UNIVERSITY CLINICAL CENTER OF VOJVODINA, NOVI SAD; (3) CLINIC OF ENDOCRINOLOGY, DIABETES AND METABOLIC DISEASES, UNIVERSITY CLINICAL CENTER OF VOJVODINA, NOVI SAD |
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
| Download in pdf format | ABSTRACT:
INTRODUCTION. Drug abuse can lead to substance-induced psychosis.
Psychotic symptoms can, as well, appear as part of the abstinence
syndrome, commonly in alcohol addiction. AIMS.Determining the
prevalence of alcohol and other substance abuse by patients
hospitalized for psychotic disorders; Determining whether there are
differences in sociodemographic, psychiatric and somatoneurological
parameters between those who used alcohol and drugs and those who
did not. MATERIAL AND METHODS. The research was conducted as a
retrospective study in which 181 patients hospitalized at the male
ward for psychotic disorders of the Clinic for Psychiatry in Novi
Sad were included. Medical documentation and clinical data grouped
into 16 variables were analyzed. The results are presented using
pictures, tables and graphs. The JMP 9 program was used for
statistical data analysis, with t-test and ꭓ2 test. Significance
level p=0.05. RESULTS. Alcohol was consumed by 41% of patients and
drugs by as many as 32% of respondents. Of the drugs, the most
prevalent was misuse of THC (13%), followed by polytoxicomania abuse
(10%), stimulants (7%) and opioids (2%), while only one respondent
was recorded as having misused hallucinogens. Abuse of THC,
stimulants and polydrug abuse are associated with younger age. The
most common somatoneurological comorbidity was hypertension.
Compliance with therapy is statistically significantly worse in the
group of alcoholics. CONLUSION. The use of alcohol and drugs is
highly prevalent in the population of male patients. Comorbid abuse
of these substances adversely affects the onset, course and
treatment of psychosis. Key words: psychosis; alcohol; psychoactive substances; opioids; hallucinogens |
|||||||||||||||||||||||||||||||||||
|
INTRODUCTION Psychosis is a condition that disrupts mental functions,
including thinking, perception, and mood, leading to a significant
reduction in social and occupational functioning [1]. Symptoms are
divided into positive (delusions, hallucinations, agitation) and
negative (social withdrawal, emotional blunting) [2], interfering
with a person's ability to think and communicate [3]. The etiology
of psychosis encompasses genetic and environmental factors, with a
significant role played by the dopaminergic and glutamatergic
systems [1,2,4]. Psychotic disorders, including schizophrenia and
schizoaffective disorder, frequently constitute the predominant
clinical presentation; however, psychotic symptoms may also manifest
in other conditions, such as those associated with substance abuse
(SA)[5-6]. Substance abuse can induce psychotic symptoms during
intoxication, particularly with hallucinogens and stimulants [8-9],
while marijuana and alcohol increase the risk of psychosis with
prolonged consumption [10-11]. Sometimes, substance-induced
psychosis develops, and in cases of persistent symptoms, they are
associated with a predisposition to psychosis [5-7]. Additionally,
withdrawal syndromes, such as delirium tremens, often include
psychotic manifestations [12]. Neurophysiological changes induced by
SA, particularly in the dopaminergic and glutamatergic systems,
explain the similarities in the pathophysiology and treatment of
induced and endogenous psychoses [4,7,13,14]. Conversely, mental
disorders often lead to substance abuse as a form of
"self-medication" [1-3,7,14], while the use of alcohol and drugs
negatively impacts the course and prognosis of psychosis [1-2,7]. MATERIAL AND METHODS The study was conducted as a retrospective study, which included
181 patients hospitalized at the male ward for psychotic disorders
at the Psychiatry Clinic in Novi Sad. Medical documentation and
clinical data of patients treated from October 1st, 2020, to October
1st, 2021, were analyzed. Since we encountered patients who were
hospitalized multiple times during this period, only the most recent
hospitalization was considered for such cases. RESULTS Out of 181 participants, data regarding the consumption of
alcohol and other psychoactive substances (PAS) were collected for
165 individuals. The most commonly consumed substance was alcohol,
reported by 41% of patients. THC, in the form of marijuana and
hashish, was used by 13% of participants. Opioids were abused by 2%
and stimulants by 7% of the participants. Among all psychoactive
substances, hallucinogens had the lowest consumption rate, with only
1% of participants using them. Polysubstance abuse was identified in
17 patients, constituting 10% of the total sample of hospitalized
individuals. A statistically significant difference (p<0.05) was
observed between the number of patients who consumed alcohol and
those who did not. Furthermore, a highly statistically significant
difference (p<0.01) was found among patients who abused THC, opioids,
stimulants and hallucinogens within their respective groups. A
significance level of p<0.01 was also observed in polysubstance
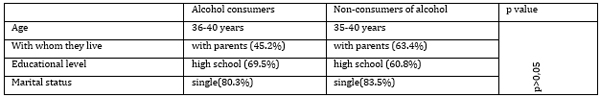
abuse. Table 1. Alcohol and Sociodemographic Parameters
A statistically significant difference (p < 0.05) was observed with regard to THC use in the younger age group.95% of those who consumed THC were aged 19-30 years. Analysis of other parameters revealed that patients in both groups most commonly lived with their parents, were single, and had a high school education (Table 2). Table 2. THC and Sociodemographic Parameters
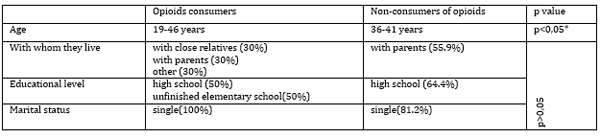
While the distribution of opioid use is associated with both adolescence and middle adulthood (95% of patients who consumed them were in the 19-46 age range), the highest percentage of those without opioid comorbidity belongs to the middle adulthood group (36-41 years). This difference was marked as statistically significant (p<0.05) (Table 3). Table 3. Opioids and Sociodemographic Parameters
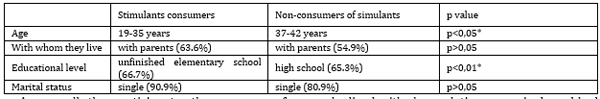
Participants in both groups are predominantly singleand live with their parents. A statistically significant difference (p<0.05) was observed in the use of stimulants, which is more common in younger age groups. Additionally, a strong statistical significance (p<0.01) was noted in the parameter 'educational level,' where the majority of consumers have not completed primary education (Table 4). Table 4. Stimulants consumers Non-consumers of simulants p value
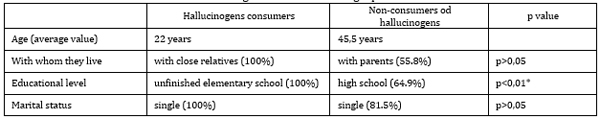
Among all the participants, the presence of hallucinogen abuse was confirmed in only one male, aged 22. His medical history indicated that he lived with close relatives, was single and had not completed primary education yet (Table 5). Table 5. Hallucinogens and Sociodemographic Parameters
Polysubstance abuse as a comorbidity in patients with schizophrenia was predominantly recorded in the age group of 20-33 years. Participants with polysubstance abuse most commonly lived with their parents (62.5%), had incomplete primary education (50%) and were single (93.8%) (Table 6). Table 6. Polysubstance Abuse and Sociodemographic Parameters
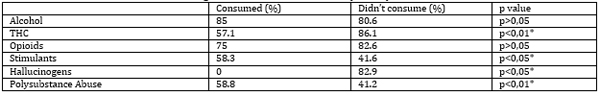
A statistically significant higher percentage of patients with a history of psychiatric treatment was observed in the groups of non-consumers of THCand individuals with polysubstance abuse (Table 7). Table 7. Percentage of Patients with a History of Psychiatric Treatment
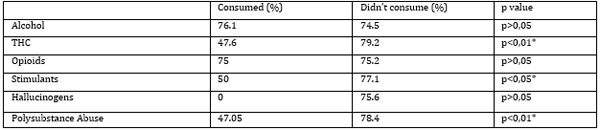
The presence of prior hospitalizations in patients was more commonly observed in the groups of those who did not consume stimulants and THC and those without polysubstance abuse (Table 8). Table 8. Percentage of Participants with a History of Prior Hospitalizations
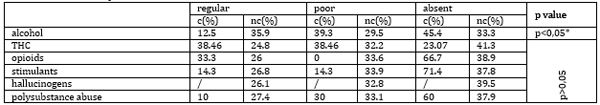
Regular compliance with medication intake was most frequently observed among hospitalized patients with THC comorbidity (38.46%) (Table 9). Table 9. Compliance with Medication and Its Association with Alcohol and Other Substance Abuse
Legend: c-consumed, nc-didn’t consume, /-without data Among individuals who consumed alcohol, 52 patients (78.78%) had no somatoneurological comorbidities, with hypertension being the most prevalent comorbid condition (observed in 5 patients, or 7.6%). In the group of THC users, hypertension, type 2 diabetes mellitus and intestinal candidiasis were equally frequent. In the opioid user group, as well as in those with polysubstance abuse, the prevalence of HIV+ status and intestinal candidiasis was identical. An analysis of participants who abused stimulants revealed the presence of HIV+ status only. No data on the presence of somatoneurological comorbidities were found for patients using hallucinogens. The majority (49.2%) of patients exhibited no psychiatric comorbidities. In the stimulant group, psychiatric comorbidities included anxiety and personality disorders. DISCUSSION The global prevalence of psychotic disorders is relatively low,
ranging from 0.2% to 3.5%. However, these disorders are more
frequently observed in impoverished areas of large cities, where
increased substance availability and consumption coincide with a
lack of adequate management due to insufficient medical oversight.
Consequently, investigating the bidirectional correlation between
psychotic disorders and substance abuse is of significant
importance. Unfortunately, it is not feasible to establish a direct
causal relationship between a specific harmful substance and the
mental state of already affected individuals, as these patients
often combine various impure chemical compounds. Substance abuse is
often driven by a variety of motivations, sometimes even simply to
mitigate the adverse effects of antipsychotic medications. Harmful
substances exert their effects by temporarily alleviating the
deficit in the dysregulated dopaminergic system, which is associated
with motivational processes and the reward system [14, 15]. CONCLUSION The study revealed that harmful use of psychoactive substances is present in 73% of patients hospitalized in psychiatry, with alcohol being the most prevalent (41%), which may be linked to cultural factors and its legal availability. Drug abuse (32%) significantly exceeds data from the general population, and the results indicate the adverse effects of drugs, particularly THC, on the early onset and severe course of psychotic disorders. Patients who abuse THC more frequently experience severe psychotic exacerbations, despite better medication adherence, which contradicts pseudoscientific claims about the "beneficial" effects of "soft" drugs. Common characteristics among patients include lower levels of education, living with parents and being single, which correlate with socio-occupational dysfunctions. The most common somatic comorbidity was hypertension, while personality and anxiety disorders were more frequent among stimulant abusers. The limitations of the study, such as the small sample size and focus on male patients with psychotic disorders, highlight the need for broader studies that would include diverse patient groups to provide a more comprehensive understanding of the relationship between psychoactive substances and psychosis. REFERENCES:
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
| [
Contents
] [ INDEX ]
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||