| |
|
|
Introduction
Meningitis represents inflammation of the meninges and, more rarely,
the brain (meningoencephalitis), characterized by the presence of
polymorphonuclear leukocytes in the cerebrospinal fluid (CSF). It is
caused by various bacteria, viruses, parasites, and other agents.
The term meningeal syndrome refers to irritation of the meninges (meningism)
or an inflammatory process affecting them (meningitis) and indicates
the need for cerebrospinal fluid puncture, which is the only method
to distinguish meningism from meningitis.
Meningism and meningitis cannot be differentiated based on clinical
presentation alone because:
There is no sign present in meningitis that does not occur in
meningism, and vice versa,
There is no difference in the intensity of meningeal symptoms in
meningitis compared to meningism,
There is no condition that could be accompanied by meningitis but
not by meningism.ETIOLOGY OF MENINGEAL SYNDROME
Meningitis can be caused by infectious agents, allergic
reactions, toxic, physical, and chemical noxae.
Bacterial meningitis is caused by pyogenic bacteria: Neisseria
meningitidis (meningococcus), Streptococcus pneumoniae (pneumococcus),
Staphylococcus, Streptococcus, Klebsiella pneumoniae, Haemophilus
influenzae, Proteus, etc.
Viral meningitis is caused by poliovirus, ECHO virus, Coxsackie
virus, Armstrong virus, mumps virus, herpes zoster, influenza virus,
mononucleosis, adenoviruses, and arboviruses.
Spirochetal and rickettsial meningitis are caused by Leptospira,
Treponema pallidum (pale spirochete), and all rickettsial species.
Fungal meningitis is typically caused by Candida.
Parasitic meningitis is caused by Ascaris, Trichinella, and
tapeworms.
Meningitis caused by chemical agents occurs due to endogenous toxins
(e.g., urea) or inhalation of toxic gases [1].
Bacterial meningitis is the most common form of infectious process
affecting the central nervous system (CNS). The incidence ranges
from 0.13 to 0.4 per 1,000 live births and is higher in preterm
infants, at 1.36–2.5 per 1,000 live births. Predisposing factors
include low gestational age, premature rupture of membranes,
cesarean section, catheterization, and prolonged rehydration.
Meningocele and spina bifida can lead to meningitis through direct
infection of the meninges [2].
Scheme 1. Classification of Meningitis
Causes [3]
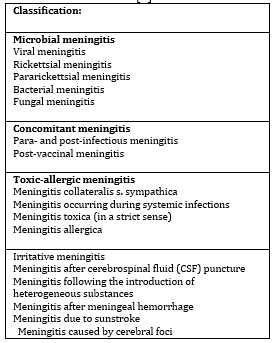
The most common causes of neonatal meningitis are Gram-negative
bacteria, with Escherichia coli (E. coli) being the most
significant. Neonatal meningitis occurs in two forms: early neonatal
meningitis, caused by Gram-positive cocci, affects 1/3 of affected
neonates. E. coli may occur sporadically or occasionally as an
epidemic in neonatal wards [3]. Other causative agents include
Proteus, Pseudomonas aeruginosa, Klebsiella, Salmonella,
Streptococcus pneumoniae (pneumococcus), and Staphylococcus, while
Neisseria meningitidis (meningococcus) and Listeria monocytogenes
are less frequently isolated. Other bacteria such as Citrobacter and
Campylobacter are rarely encountered [3,4].
PATHOANATOMICAL CHANGES IN MENINGEAL SYNDROME
In purulent meningitis, changes occur in the meninges with the
accumulation of purulent exudate in the subarachnoid space and
ventricles. This leads to increased intracranial pressure and
sometimes to ventricular occlusion, which may cause pyocéphaly.
Purulent exudate accumulates at the base of the brain and on the
convexities, commonly in pneumococcal meningitis. Inflammation can
affect cranial nerves, causing blindness, deafness, or paralysis.
Endotoxin from meningococcus causes thrombosis, hemorrhages, and
perivascular infiltrates, leading to degenerative changes in organs
and tissues, particularly in the skin, brain, and adrenal glands.
Brain edema may occur due to decreased cerebrospinal fluid pH and
bacterial toxic factors, resulting in ischemia and altered
consciousness. The exudate may organize, forming adhesions that can
cause hydrocephalus [5].
PATHOGENESIS OF MENINGEAL SYNDROME
Bacteria such as Neisseria meningitidis, Haemophilus influenzae,
Streptococcus pneumoniae, and E. coli evade the body's defense
mechanisms by adhering to mucosal cells. The bacterial capsular
polysaccharide prevents phagocytosis, allowing bacteria to avoid the
complement system. After surviving in the intravascular space,
bacteria enter the subarachnoid space, where the body's defenses are
insufficient.
Inflammation in the subarachnoid space leads to increased complement
levels in the cerebrospinal fluid, while immunoglobulin
concentrations remain low, contributing to the immune deficiency in
this space during bacterial meningitis [5].
PATHOPHYSIOLOGY OF MENINGEAL SYNDROME
In experimentally induced infections, subcapsular components of
bacteria (cell wall and lipopolysaccharide or endotoxin) are
significant determinants of pathogenicity compared to surface
components. For example, in the cell wall of Streptococcus
pneumoniae, two main polymers are present: peptidoglycan and ribitol-phosphate
teichoic acid. The former causes inflammation within 24 hours, while
the latter does so within 5 hours [5].
Blood-Brain Barrier (BBB) Damage
The blood-brain barrier (BBB) separates cerebrospinal fluid and
brain tissue from the intravascular space. The main sites are the
arachnoid membrane, the epithelial layer of the choroid plexus, and
the endothelium of cerebral capillaries. These capillaries are the
primary sites of damage due to the endothelium's unique
ultrastructural properties—sparse plasmalemmal vesicles and
continuous intracellular tight junctions, which make them resistant
[5,6].
Interaction Between Leukocytes and Endothelial Cells
An essential component of the inflammatory response during bacterial
meningitis is the migration of circulating leukocytes, primarily
neutrophils, from the bloodstream into the cerebrospinal fluid. This
process depends on interactions between endothelial cells and
leukocytes.
During acute inflammation, circulating leukocytes are activated by
various inflammatory mediators, such as complement components,
cytokines, and bacterial lipopolysaccharide. This activation leads
to leukocyte sequestration in the microcirculation, partly due to
reduced deformability and increased endothelial adhesiveness [5].
Changes in Intracranial Pressure and Cerebral Blood Flow
Intracranial pressure (ICP) is often elevated during bacterial
meningitis and may cause cerebral herniation, which is
life-threatening. During the early hours of infection, cerebral
blood flow (CBF) increases by 100–200%, which, along with brain
edema, leads to intracranial hypertension.
As the infection progresses, cerebral blood flow decreases while ICP
continues to rise, and vasculitis develops. In approximately 30% of
infants and children with bacterial meningitis, cerebral blood flow
is reduced by 30–70%. Factors explaining the association between
reduced cerebral blood flow and poor outcomes include inadequate
delivery of energy substrates, increased metabolic demands, or
inefficient substrate utilization.
Metabolic encephalopathy is believed to result from free radicals,
endotoxins, prostaglandins, or other neurotoxins released during
infection. Brain edema correlates with the degree of protein in
cerebrospinal fluid (proteinorachia) but may also occur due to
hyponatremia, which results from inappropriate antidiuretic hormone
secretion [5].
Outcome of Bacterial Meningitis
The outcome of bacterial meningitis depends on cerebral perfusion
pressure (CPP). The highest morbidity and mortality are observed in
children with CPP below 30–50 mmHg.
Image 1. Pathophysiology of Bacterial
Meningitis [3]
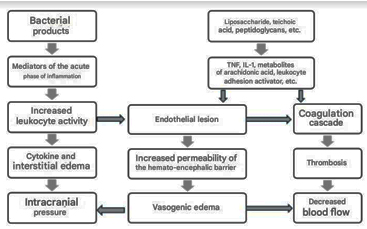
CLINICAL PICTURE
Meningitis cerebrospinalis epidemica
The clinical manifestations of bacterial meningitis in newborns are
not characteristic.
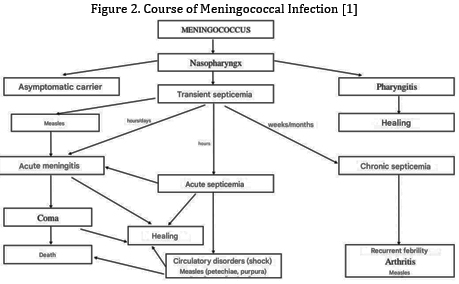
Scheme 2. Symptomatology of Meningitis [2]

Symptomatology of meningitis encompasses three main syndromes:
infectious, meningeal, and cerebrospinal fluid (CSF) syndromes.
INFECTIOUS SYNDROME
Initial symptoms include fatigue, general weakness, and anorexia.
MENINGEAL SYNDROME
This syndrome arises due to increased intracranial pressure and
develops rapidly (within 1-3 days). Clinical manifestations include:
Headache – Intense and persistent, unrelieved by analgesics.
In children, manifests as restlessness, crying, and constant head
movement.
Vomiting – No relief after vomiting; referred to as "central
vomiting."
Fontanelle tension – Increased intracranial pressure in
infants with an open fontanelle.
Meningeal signs – Neck stiffness, Kernig's sign, Brudzinski's
sign; reflexes due to pressure on the brain.
Increased sensitivity – Photophobia, hyperacusis, painful
palpation of muscles.
Neurovegetative disorders – Cerebral vomiting, bradycardia,
constipation, pronounced dermographism.
Altered consciousness – Ranges from drowsiness to coma,
caused by fever, inflammation, edema, and intracranial pressure.
CEREBROSPINAL FLUID (CSF) SYNDROME
This includes changes in CSF accompanying acute leptomeningeal
inflammation:
Clear CSF – Normal, as in serous meningitis, with a positive
Pandy's reaction.
Cloudy CSF – Indicates purulent meningitis.
DIAGNOSIS OF MENINGEAL SYNDROME
The diagnosis of neonatal meningitis is established through
medical history, clinical examination, and laboratory tests,
primarily lumbar puncture. The cerebrospinal fluid (CSF) analysis
includes:
- White blood cell count in CSF,
- Differentiation of cellular elements,
- Preliminary protein level determination using Pandy's
reagent,
- Microscopic examination of Gram-stained CSF,
- Microscopic examination of CSF sediment,
- Glucose levels in CSF and blood,
- Quantitative protein analysis in CSF,
- CSF culture.
- Other laboratory tests include:
- Fundoscopic examination,
- EEG,
- Brain ultrasound (ECHO),
- Stool culture,
- Urine culture,
- Blood culture,
- Throat swab,
- Complete blood count,
- Erythrocyte sedimentation rate,
- Ionogram,
- C-reactive protein.
Additional methods such as immunoelectrophoresis, latex
agglutination, ELISA test, and Limulus test can also be used. The
diagnosis is based on the clinical presentation and CSF findings
from lumbar puncture, where the CSF is typically cloudy. The primary
method for bacterial detection is the microscopic examination of
Gram-stained CSF sediment.
Table 1. Characteristics of Normal
Cerebrospinal Fluid and Cerebrospinal Fluid from Patients with
Different Types of Meningitis [3]
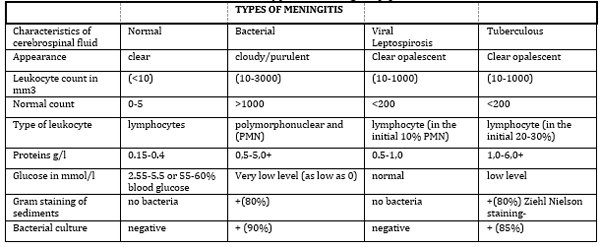
Differential Diagnosis
In the differential diagnosis of bacterial meningitis, the following
diseases are considered:
- Viral meningitis
- Tuberculous meningitis
- Leptospirosis meningitis
- Fungal meningitis
- Parasitic meningitis
- Brain abscess
- Brain tumor
- Ruptured blood vessel
- Febrile convulsions, and others
I8. Complications of Meningeal Syndrome
Complications of meningitis may include:
- Subdural effusion (fluid accumulation in the subdural space,
manifesting with fever, convulsions, somnolence, agitation,
tense fontanelle, etc.)
- Ventriculitis
- Abscess formation or hydrocephalus
- Damage to cranial and/or spinal nerves
Prognosis of Bacterial Meningitis
The prognosis of acute bacterial meningitis depends on six key
factors: the child's age, type of bacteria, speed of diagnosis,
consciousness level, presence of convulsions, and serious mechanical
complications. Pneumococcal meningitis has a higher chance of
complications and a higher mortality rate (20%) compared to
meningococcal and Haemophilus influenzae meningitis (5-10%). The
mortality rate is 40-60% in neonates, while neurological
consequences (hydrocephalus, convulsions, psychomotor retardation,
etc.) are registered in 31-56% of surviving children.
Viral Meningitis
Etiology
Viral meningitis is most commonly caused by enteroviruses (ECHO and
Coxsackie viruses), mumps virus, and less commonly by viruses such
as lymphocytic choriomeningitis (LCM), herpes virus, adenovirus,
cytomegalovirus, Epstein-Barr virus, Herpes-zoster virus, influenza
virus, measles, rubella, and arboviruses. In our country, the most
common pathogens are enteroviruses and the mumps virus. Viral
meningitis accounts for 60-70% of all meningitis cases.
Enteroviruses are transmitted fecal-orally, usually during the
summer months, and primarily affect children up to 10 years old. The
mumps virus is transmitted by droplets, causing epidemics every 3-4
years, most commonly in children between 5-12 years. Lymphocytic
choriomeningitis virus occurs sporadically, mostly in winter months,
and is transmitted from rodents. Chronic serous meningitis can also
be caused by pale treponema, fungi, parasites, and neoplasms.
2. Pathogenesis and Pathoanatomic Changes
Enteroviruses reach the meninges via viremia, while the mumps virus
enters the body through the nasopharyngeal mucosa and then spreads
through the bloodstream to the CNS. Pathohistological changes in
organs are not well known due to the good prognosis of viral
meningitis.
3. Clinical Picture of Viral Meningitis
Symptoms are often milder than those of bacterial meningitis, and
the incubation period depends on the virus type. The disease may
begin abruptly with symptoms such as headache, chills, malaise,
abdominal pain, leg and back pain, vomiting, and fever. Meningeal
symptoms like neck stiffness and a positive Kernig's sign are
present but less pronounced than in bacterial meningitis.
Additionally, enteroviral meningitis may cause lymphadenitis,
pharyngitis, conjunctivitis, and rash in children under 3 years old.
Mumps meningitis is typically associated with parotitis. In rare
cases, convulsions or meningoencephalitis may occur during viral
meningitis. Recovery is usually complete, though symptoms may last
several weeks.
4. Diagnosis of Viral Meningitis
The diagnosis is based on the clinical picture, epidemiological
data, and cerebrospinal fluid (CSF) analysis. The CSF is clear, with
leukocyte counts ranging from 100 to 1000 per mm³, and elevated
protein levels are present along with normal glucose levels.
Specific findings may include the presence of lymphocytes in the
CSF. For etiology diagnosis, virus isolation from CSF, throat swab,
or stool, or a rise in antibody titers may be used. Peripheral blood
may show leukocytosis with lymphocytosis.
5. Treatment of Viral Meningitis
The treatment is primarily symptomatic, including analgesics,
antipyretics, antiemetics, and infusions. Main therapeutic measures
include:
Fluid intake: Initial fluid intake should be 800-1000 mL/m²
body surface area, and it should be gradually increased. If sodium
levels are low, diuretics and sodium chloride are used.
Intracranial hypertension treatment: This includes general
and specific measures, such as raising the head by 30°, and using
mannitol (0.5-2.0 g/kg) to reduce pressure.
Seizure treatment: Diazepam (0.25-0.5 mg/kg i.v.) is used to
stop seizures, along with phenytoin or phenobarbital for
anticonvulsant effects.
Infants, Toddlers, Preschool and School-Age Children
Etiology and Pathogenesis
Purulent meningitis in children of this age group is usually caused
by Neisseria meningitidis (meningococcus), Streptococcus pneumoniae
(pneumococcus), and Haemophilus influenzae. Less common pathogens
include Staphylococcus aureus, Proteus mirabilis, Pseudomonas
aeruginosa, Listeria monocytogenes, Klebsiella, and others.
Meningitis may result from the direct spread of bacteria from nearby
inflamed sites, such as otitis, sinusitis, or otitis media.
Meningococcus most commonly enters the body via droplets through the
nasopharynx, where it may remain latent or cause nasopharyngitis,
which spontaneously resolves after a few weeks. In some cases,
meningococcus enters the bloodstream and causes bacteremia, which
may progress to meningitis by crossing the blood-brain barrier.
Clinical Picture
Infants: Meningitis may start abruptly with convulsions or coma,
although it often begins gradually. The child becomes febrile,
lethargic, irritable, refuses to feed, vomits, has diarrhea, and
often becomes dehydrated. Neck stiffness may be mild, and hypotonia
is common, with the head often falling backward. The key sign is a
"tense fontanelle," indicating increased intracranial pressure.
Other signs may include vasomotor disturbances like pale or flushed
face, spleen swelling, joint swelling, and petechiae.
Preschool and school-age children: Meningitis often begins abruptly
with high fever (39-40°C), headache, and vomiting. The headache
becomes severe and worsens with head movements. Vomiting is
frequent, and the patient complains of malaise, muscle, and joint
pain. As the disease progresses, meningeal symptoms appear: neck
stiffness, increased sensitivity to light (photophobia), hyperacusia,
irritability, and the presence of reflexes such as Kernig's and
Brudzinski's signs. In some cases, somnolence, stupor, or coma may
develop. Bradycardia, dermographism, and hyperactive tendon reflexes
may also be present. If the condition worsens, cranial nerve
paralysis or a positive Babinski sign may occur. In 20-30% of cases,
febrile herpes appears, which has diagnostic significance in
epidemic meningitis.
Diagnosis and Treatment
The diagnosis and treatment of meningitis in this age group depend
on the exact identification of the pathogen and prompt initiation of
therapy.
1. Therapy for Infants Aged 29 to 60 Days
Due to the unpredictability of bacterial meningitis pathogens in
infants of this age, treatment should start with a three-component
therapy before the pathogen is identified. The recommended drug
combination includes:
Ampicillin – for controlling infections caused by Listeria
monocytogenes and Streptococcus agalactiae
Amikacin – for its effectiveness against gram-negative
bacteria
Chloramphenicol – which covers many bacteria, including
Haemophilus influenzae and Streptococcus pneumoniae
This combination provides broad-spectrum protection until the
specific pathogen is identified.
Therapy for Infants Over 2 Months, Preschool, and School-Age
Children
For children older than 2 months, a combination of penicillin and
chloramphenicol is commonly used, while newer cephalosporins are
indicated in cases where bacterial resistance is identified
(particularly against Haemophilus influenzae and Streptococcus
pneumoniae).
Benzylpenicillin G: 400,000 IU/kg or 10,000,000 IU/m daily,
divided into 8-12 doses or continuously via infusion.
Chloramphenicol succinate: 2.5 g/m² daily, divided into 4-6
doses.
2. Therapy for Purulent Meningitis
Treatment for purulent meningitis requires immediate administration
of antibiotics and symptomatic therapy. Antibiotic therapy should
begin immediately after blood and CSF samples are taken.
Meningococcal meningitis: The drug of choice is Penicillin
G, administered intravenously in infusions, in a dose of 300,000
IU/kg/day divided into 6 doses over 7 days. If resistance or
hypersensitivity to penicillin exists, third-generation
cephalosporins (e.g., cefotaxime) or chloramphenicol should be used.
Haemophilus influenzae: The preferred treatment for purulent
meningitis caused by H. influenzae is chloramphenicol, which can be
used alone or in combination with ampicillin, at doses of 300-400
mg/kg/day, divided into 4-6 doses for 10-14 days.
Gram-negative bacteria: For meningitis caused by
gram-negative bacteria, second-generation cephalosporins are more
effective than aminoglycosides or ampicillin.
Symptomatic therapy includes:
Fluid and electrolyte replacement via saline.
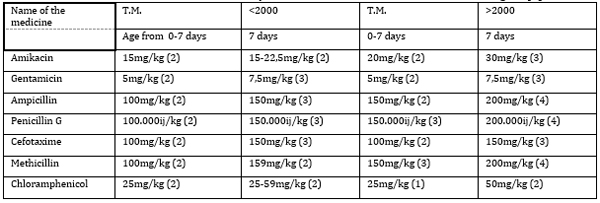
Table 2. Antibiotics Most Commonly Used in
the Treatment of Neonatal Meningitis [3]
CONCLUSION
Based on the presented facts and data, we can conclude the
following:
Purulent meningitis is a disease that is widespread worldwide,
occurring sporadically, except when caused by meningococcus, which
can appear endemically and epidemically.
Epidemics are usually caused by meningococcus group A, and they most
commonly occur at the end of winter and the beginning of spring.
The source of infection is more often a healthy carrier (about 10%
of the general population are healthy carriers, and among those who
have been in contact with individuals suffering from meningeal
meningitis, this percentage is higher, around 25%), and less
frequently a patient.
Viral meningitis is usually a disease of school-age children and
younger individuals.
Serous meningitis is usually a disease of school-age children and
younger individuals.
Tuberculous meningitis always ends in death if treatment is delayed.
Clinical study results have shown that early adjuvant therapy with
dexamethasone significantly reduces the frequency of neurological
sequelae in affected children.
The most commonly used therapy is penicillin, followed by
third-generation cephalosporins or chloramphenicol.
The fatal outcome occurs in 40 to 60% of affected neonates, while
neurological sequelae are observed in 31 to 56% of surviving
children.
Based on all the above, we can conclude that meningeal syndrome
represents a significant practical and theoretical problem that
requires extensive epidemiological and clinical investigations.
LITERATURE:
- Problemi u pedijatriji 2022. Zbornik, Medicinski fakultet
Beograd, 2022; 52:76-93.
- Wadsworth AW, Garvey KL, Goodman DM, Landerdare DS, The
Journal of Pediatrics. 2023; 254-260.e1.
- Kolar J. Neurologija. Stomatološki fakultet u Pančevu. 2021;
10:110-2.
- Kostić V. Neurology for Medical Students. 2024; 7:120-43.
- Problemi u pedijatriji 2023.Zbornik, Medicinski fakultet
Beograd, 2023; 70:93-110.
- Božić M. Infektivne bolesti, Naučna knjiga Beograd, 2021;
10:68/13.
- Ropper A.H, Samuels M.A, Klein J.P., Prasad S. Principles of
neurology 12e. Adams and Victor's. 2023.
- Bašić-Kes V. Hitna stanja u neurologiji. Medicinska –
Naklada 2024.
|
|
|
|






