|
||||||||||||||||||||||||||||||||||||
| [
Contents
] [ INDEX ]
|
||||||||||||||||||||||||||||||||||||
|
Page 45 |
||||||||||||||||||||||||||||||||||||
|
Case report Myocardial infarction with non-obstructive coronary artery disease (MINOCA) - Case report Danijela Ćirić GENERAL MEDICINE, HEALTH CENTER ZAJECAR, ZAJECAR
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
| Download in pdf format | Summary:
Introduction: Acute coronary syndrome type myocardial infarction
with non-obstructive coronary artery disease (MINOCA) represents a
myocardial infarction without coronary artery stenosis or with
stenosis less than 50%. The aim of this paper is to highlight MINOCA
as a relatively new entity in cardiology, the importance of early
diagnosis and timely treatment, as well as the application of
primary and secondary prevention of cardiovascular diseases along
with the modification of risk factors for these conditions. Case
presentation: A 60-year-old female patient presents with chest pain
described as tightness and pressure. The physical examination is
normal, while the electrocardiogram shows ST-segment depressions in
leads V4-V6 ranging from 0.5 mm to 1 mm. The patient was treated
according to the protocol for non-ST-elevation myocardial infarction
(NSTEMI). Coronary angiography was immediately performed and found
to be normal. Treatment was continued with medical therapy.
Conclusion: MINOCA encompasses a heterogeneous group of patients who
experience myocardial infarction but do not have significant
coronary artery obstruction on angiogram. Our patient had a typical
presentation of non-ST-elevation infarction and was treated with
medical therapy to reduce cardiovascular risk for future events and
improve outcomes. Key words: Acute coronary syndrome (ACS), Myocardial infarction without persistent ST elevation (NSTEMI), Prevention, Myocardial infarction with non-obstructive coronary artery disease (MINOCA), Treatment, Prevention |
|||||||||||||||||||||||||||||||||||
|
INTRODUCTION Acute coronary syndrome (ACS) accounted for
48.3% of all deaths from ischemic heart diseases in Serbia in 2022.
According to data from the population registry for ACS, in 2022, the
diagnosis of acute coronary syndrome was made in 19,701 cases in
Serbia. During 2022, 4,564 people in Serbia died from this syndrome.
Myocardial infarction with non-occlusive coronary arteries (MINOCA)
refers to a clinical situation in which a patient exhibits symptoms
suggestive of acute coronary syndrome (ACS), with elevated troponin
levels, but coronary angiography shows no significant obstruction of
the coronary arteries (defined as stenosis <50% in any major
epicardial artery). The reported prevalence of MINOCA significantly
varies in different studies, ranging from approximately 1% to 14% of
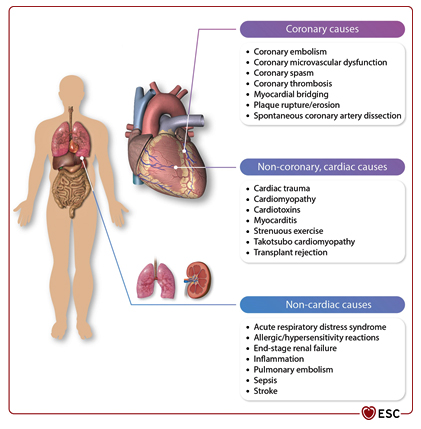
ACS patients undergoing angiography [1]. Figure 1. MINOCA - a common term
encompassing a heterogeneous group of coronary and non-coronary
causes.
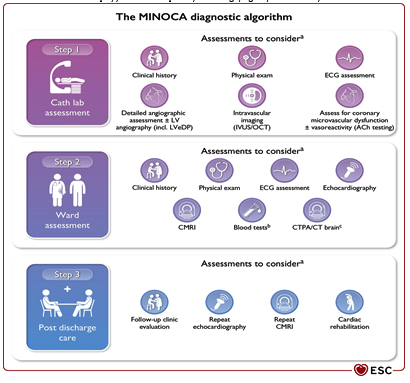
When the diagnosis is not clearly established after coronary angiography, MINOCA represents a working, rather than a final, diagnosis. It is crucial that clinicians conduct additional assessments and investigations to identify the underlying cause of MINOCA, which will enable a definitive diagnosis and appropriate treatment for the patient. Failure to identify the underlying cause of MINOCA may lead to inadequate or inappropriate therapy [1]. If the underlying cause of MINOCA cannot be determined solely through invasive coronary angiography (ICA), further assessments of microvascular function and coronary artery reactivity, as well as intravascular imaging, should follow. The term "functional coronary angiography" refers to the combination of standard coronary angiography with additional tests (e.g., testing for coronary microcirculation dysfunction and vasoreactivity) (Figure 2). Figure 2. MINOCA diagnostic algorithm.
Evaluation of patients with a working diagnosis of MINOCA.
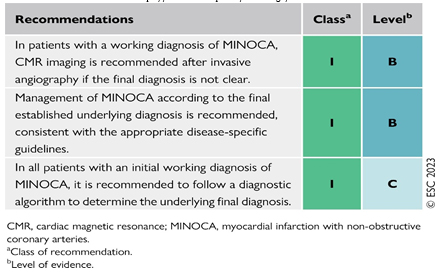
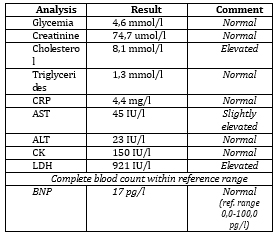
If the underlying cause of MINOCA cannot be determined through functional coronary angiography, non-invasive imaging is recommended (e.g., echocardiography, CMR, CT angiography, CT heart), according to the clinical indication. Cardiac magnetic resonance (CMR) is one of the key diagnostic tools for determining the underlying cause of MINOCA [7–11]. CMR can identify the underlying cause in up to 87% of patients with a working diagnosis of MINOCA and should be performed as soon as possible after patient admission, ideally during the initial hospitalization [12]. (Table 1) Table 1. Recommendations for myocardial
infarction with non-occlusive coronary arteries (MINOCA)
Determining the underlying cause of MINOCA enables the initiation
of appropriate therapy in accordance with the final diagnosis.
Secondary preventive therapy should be considered for patients with
evidence of coronary atherosclerotic disease and for the control of
risk factors. CASE REPORT A 60-year-old female patient presents with chest pain described
as tightness and pressure at rest. She reports that the day before
seeing the doctor, she felt chest pain resembling tightness and
pressure. The pain occurs with exertion, most often when walking
uphill, lasts longer than half an hour, radiates through the left
side of the chest, and decreases with cessation of exertion, which
corresponds to the clinical picture of unstable angina pectoris. She
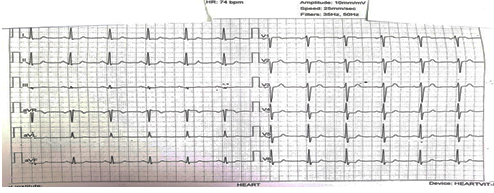
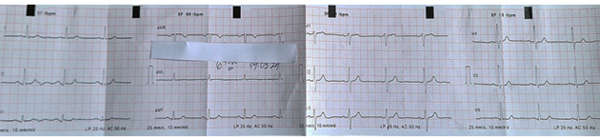
had no similar symptoms previously. Figure 3. Electrocardiogram of the patient upon admission
The patient was admitted with a diagnosis of acute coronary
syndrome type unstable angina, and during hospitalization, the first
cardiac biomarker, high-sensitivity troponin (hs-cTnI), was 4.3 ng/l,
which was normal. The following day, hs-cTnI was repeated and found
to be 79.2 ng/l, showing an increase of approximately 20 times from
the first value, and 7 times higher than the upper reference limit
(reference range 0.0-11.6 ng/l), which led to the definitive
diagnosis of non-ST-elevation myocardial infarction.
Treated according to the NSTEMI protocol. The therapy included
low-molecular-weight heparin, dual antiplatelet therapy (DAPT), the
beta-blocker nebivolol, ACE inhibitor, calcium channel blocker,
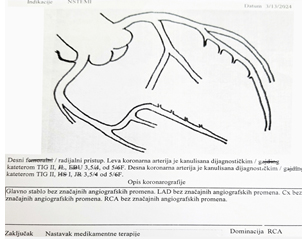
diuretic, proton pump inhibitor, and nitroglycerin as needed. Figure 4. Coronary angiography report
Given the absence of significant stenosis, medical and
pharmacological therapy was continued. During the further course of
hospitalization, to determine the cause of MINOCA, an echocardiogram
was performed: concentric hypertrophy of the left ventricular walls,
with normal systolic function, ejection fraction (EF) = 60%, without
clear segmental abnormalities in contractility, which excludes a
large infarction and supports the possibility of a subendocardial
infarction in the presence of myocardial hypertrophy. Figure 5. ECG of the patient at discharge
Therapy at Discharge: DAPT, beta blocker nebivolol; ACE inhibitor, calcium channel blocker and diuretic as a fixed combination, proton pump inhibitor, and nitroglycerin as needed. DISCUSSION According to the fourth universal definition of myocardial
infarction, there are several subtypes of myocardial infarction.
There is a group of patients with MI without angiographically
obstructive coronary artery disease (without stenosis of 50% or more
in a large epicardial vessel), and the term myocardial infarction
without coronary artery obstruction (MINOCA) has been adopted for
this entity. Prevalence is estimated at 6-8% [4], but it is
heterogeneous and varies from 1% to 14% of patients with ACS [1].
MINOCA is more common in women, as well as in patients presenting as
NSTEMI [4]. The criteria for diagnosing MINOCA are: CONCLUSION Myocardial infarction with non-obstructive coronary artery disease (MINOCA) is a relatively new entity in cardiology and encompasses a heterogeneous group of patients who do not have significant coronary artery obstruction on angiography. The aim of this paper is to highlight MINOCA as a relatively new entity in cardiology, the importance of early diagnosis and timely treatment, as well as the application of primary and secondary prevention of cardiovascular diseases with modification of risk factors. The presented patient, based on the symptoms of angina and ST segment depression on the ECG, was initially diagnosed as a classic acute coronary syndrome without persistent ST elevation but with significantly elevated troponin levels, as a myocardial infarction with probable severe coronary stenosis or occlusion. However, the normal coronary angiography result classified her into the relatively rare MINOCA group. The patient was treated according to the acute coronary syndrome protocol, and during the course of hospitalization, there were no complications. She was discharged for further home treatment with pharmacological therapy, including dual antiplatelet therapy, and advice on hygiene-dietary measures to modify risk factors. The patient was advised to have regular check-ups and was referred for cardiac magnetic resonance imaging, which, according to the MINOCA algorithm, would clarify the cause of the infarction. REFERENCE:
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
| [
Contents
] [ INDEX ]
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||